Lauren Sharkey
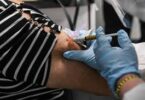
WASHINGTON: Keeping blood glucose at a healthy level reduces the risk of developing diabetes. But until now, reducing high glucose levels has focused on limiting carb and calorie intake, rather than on how individuals respond to different foods.
Health meal together
The number of people in the United States who receive a diagnosis of diabetes continues to rise.
According to the Centers for Disease Control and Prevention (CDC), 9.4 percent of the U.S. population had diabetes in 2015.
Some sources estimate that about 40 percent of U.S. adults have prediabetes. This condition is characterized by higher than normal blood sugar levels and may lead to type 2 diabetes, heart disease, and stroke.
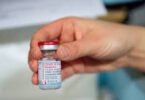
Experts are always looking for ways to prevent the onset of the condition. Reducing blood sugar — or blood glucose — levels is the primary method.
Typically, this involves controlling diet with a specific focus on lowering calorie and carbohydrate intake. Not only can this prevent diabetes, but it can also reduce a person’s risk of obesity and heart or kidney disease.
However, new research has shown that taking a more individualized approach may produce better results. “The current models of predicting blood glucose levels perform well, but they tend to bucket everything, like fats and carbohydrates, into one category,” says Purna Kashyap, co-director of the Mayo Clinic Center for Individualized Medicine Microbiome Program, in Rochester, MN.
“As a clinician, I have seen that my patients do not respond to the same foods the same way — just like not all weight-loss diets work for all people the same,” adds study co-author Dr. Heidi Nelson.
The influence of the microbiome
The research team worked to find a model that could predict how blood sugar levels would react after a person ate specific foods.
The team took individual features into account. These included age, diet, and physical activity. They also considered the gut microbiome — the trillions of bacteria living in the intestines.
In total, 327 people living in either Minnesota or Florida took part in the study. Each participant gave a stool sample, which allowed researchers to examine each person’s unique gut microbiome. The team followed the participants for 6 days.
For breakfast, the volunteers ate bagels and cream cheese. The participants were then free to choose their diet for the rest of the day. The researchers asked them to record everything they ate, along with any exercise and rest periods. A blood glucose monitor also tracked blood sugar levels every 5 minutes.
The results are available in the JAMA Network Open journal. The article reports that the newly developed model accurately predicted how blood sugar responded to food 62 percent of the time.
Researchers noted that this was a significant improvement compared to the accuracy based on just carbohydrates (40 percent) or calories (32 percent).
Additionally, the team was able to see why certain foods resulted in tiredness for some people but gave others more energy.
“For people who want to manage their blood glucose levels, we have a new model that predicts their unique response to foods.”
Strengthening the case
Many studies on the topic tend to rely on self-reported data. This can be a problem if a person does not report elements of their day-to-day life accurately.
However, in this particular study, the researchers provided the participants with a food-logging app that allowed them to log meals instantly and privately, reducing the chance of forgetfulness.
It is not the only study to promote a different take on managing blood sugar levels. A 2015 study conducted at Israel’s Weizmann Institute of Science demonstrated similar findings.
The research team believes that comparable findings from two different countries strengthen the case for the individualized model.
“The similarity of results across Israel and the United States suggests that the individualized model works across diverse populations, despite personal traits and microbiomes that tend to vary due to different geographic locations, genetics, and behaviors.”
Courtesy: (medicalnewstoday)