F.P. Report
ISLAMABAD: The number of daily coronavirus infections remained low again as Pakistan recorded 48 Covid-19 cases and no death during the last 24 hours (Sunday), showed the figures released by the National Institute of Health Pakistan on Monday morning.
As per the latest NIH data, the death toll remained the same at 30,379, whereas the number of total infections now stood at 1,530,333 after adding the fresh 48 cases.
During the last 24 hours (Sunday), 12,866 tests were conducted throughout Pakistan whereas the positivity ratio stood at 0.37 percent. The number of patients in critical care was recorded at 75.
During the last 24 hours (Sunday), another 93 people recovered from the Covid-19 and the number of total recoveries now stood at 1,496,575. As of Monday, the total count of active cases in the country was recorded at 3,379.
As many as 577,517 coronavirus cases have so far been confirmed in Sindh, 507,157 in Punjab, 219,681 in Khyber Pakhtunkhwa, 135,396 in Islamabad, 35,501 in Balochistan, 43,332 in Azad Kashmir and 11,749 in Gilgit-Baltistan.
As many as 13,564 individuals have lost their lives to the pandemic in Punjab so far, 8,106 in Sindh, 6,324 in KP, 1,024 in Islamabad, 792 in Azad Kashmir, 378 in Balochistan and 191 in Gilgit Baltistan.
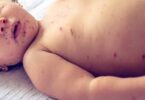
New Covid study charts evolution of symptoms
A yearlong study of more than 60,000 people tested for the coronavirus in San Francisco found intriguing shifts in COVID-19 symptoms over three different surges — including fewer reports of loss of smell, once considered a trademark of the illness — probably because of changes in the virus itself as well as individuals’ immunity.
More people with COVID reported symptoms of upper respiratory infection — including cough, sore throat and congestion — during the omicron surge than earlier waves, researchers found. Patients also experienced fewer instances of systemic issues such as fever and body aches. Loss of smell was reported by 20% of those who tested positive during the delta surge, but only 5% during omicron.
The same study, which has not yet been peer-reviewed, also found that most people infected during the omicron surge tested positive for at least five days, and in many cases up to 10 days, after their first positive test. This suggests they may remain infectious for several days after their symptoms have improved or gone away entirely, well after federal guidelines state they no longer need to isolate. California guidelines are more restrictive and recommend isolating as long as people test positive, for up to 10 days.
The findings demonstrate how COVID has become milder for many people over time, but also underscore the ways in which it remains a threat that’s stubbornly difficult to control, especially as more blunt mitigation measures such as mask mandates are no longer in place and programs to support those who are ill fade away, health experts said.
“Milder illness does not mean no illness,” said Dr. Diane Havlir, a UCSF infectious disease expert and senior author of the study. “It does not mean the illness doesn’t affect people’s ability to go to work and support their families. And we’re still seeing hospitalizations. We are still in a pandemic, and we need to keep our response on pace with the virus.”
The San Francisco study was conducted by researchers at UCSF and the Chan Zuckerberg Biohub in coordination with the San Francisco Latino Task Force. They looked at people who got tested at the Unidos en Salud testing site in the Mission District from January 2021 to January this year.
That period included three surges: the first fuelled by the epsilon and alpha variants, the second by delta, and the third by omicron.
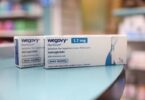
Pfizer to sell low-cost drugs to poor countries
The drug company Pfizer will make all of its patented medicines available at a not-for-profit price to 45 of the poorest countries.
The company announced the effort at the recent World Economic Forum in Davos, Switzerland. Pfizer is calling it “An Accord for a Healthier World.” It said new medicines and vaccines would be added to the list at not-for-profit prices when they are launched.
The drugs include COVID-19 treatment Paxlovid and breast cancer drug Ibrance, the drugmaker said on Wednesday.
The Bill & Melinda Gates Foundation said it can take four to seven years or longer for new treatments to become available in poor countries. Sometimes they do not become available at all.
Pfizer said its plan includes 23 patented medicines and vaccines that the company fully owns. The medicines treat infectious diseases, some cancers, and rare and inflammatory diseases. In addition to Paxlovid and Ibrance, the list includes pneumonia vaccine Prevnar 13, rheumatoid arthritis drug Xeljanz and cancer treatments Xalkori and Inlyta.
The COVID-19 vaccine Comirnaty developed with the German company BioNTech is also on the list.
Pfizer’s Chief Executive Officer Albert Bourla said that all the medicines being made available should be of use. “But clearly the antiviral Paxlovid is going to be a very big deal for them – if they need it they can get it immediately,” he said.
The 27 low-income countries and 18 lower-income countries included in the deal cover most of Africa and much of Southeast Asia. Five countries – Rwanda, Ghana, Malawi, Senegal and Uganda – have already agreed to join.
Malawi’s President Lazarus Chakwera made a statement about the agreement. He said it will let the countries and the drugmaker share “the burden of costs and tasks in the production and delivery of supplies that will save millions of lives.”
Pfizer has been criticized for how it made its COVID-19 vaccine available. Some poor countries waited for months after the approval of the vaccine in rich countries.
Bourla said the new agreement uses information learned during the release of the vaccine. He added that the lack of health systems in some countries made providing the vaccine to people who needed it difficult.
To avoid that, Bourla said the agreement not only supplies the treatments, it will also help organize a system to administer them.